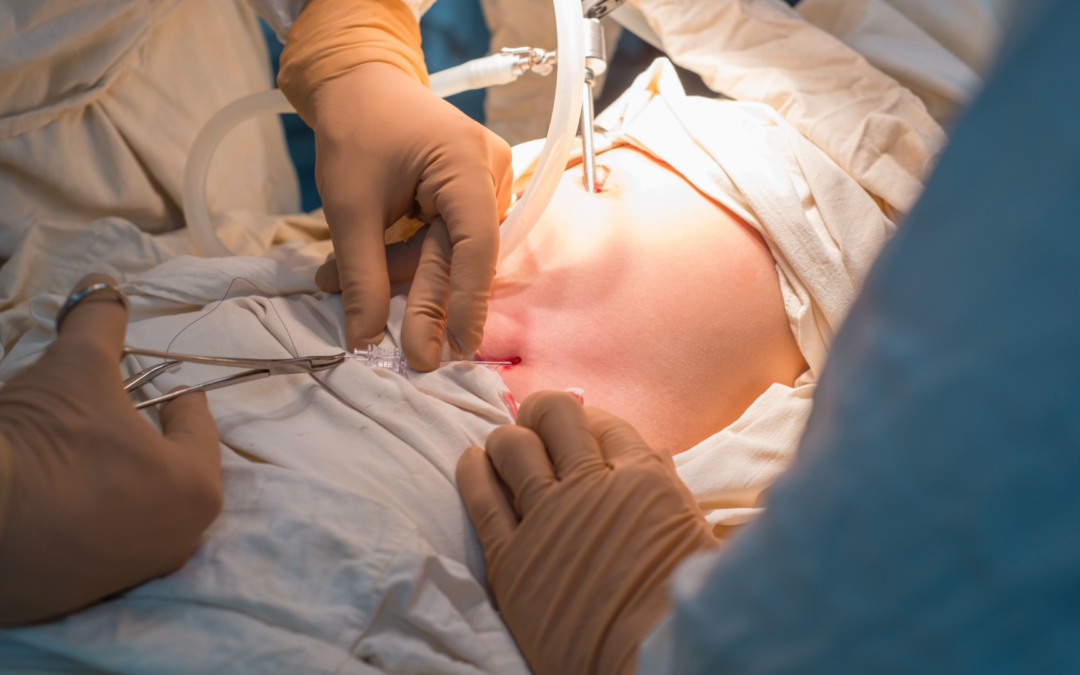
According to Dr. Sandeep Nayak, Surgical oncologist in Bangalore,
“I switched to laparoscopic years ago because watching patients struggle through open surgery recovery when something better existed didn’t sit right with me anymore.”
What Physical Symptoms Suggest Cancer Has Come Back
- Incision size: Open leaves a 15-30 cm wound. Takes weeks to close, months before your abdominal wall feels like it belongs to you again. Laparoscopic uses 3-4 tiny ports. Less tissue torn apart. Less pain. Less scarring. Fewer wound problems. Pretty straightforward math.
- Recovery speed: Open patients sit in hospital 7-14 days then another 6-8 weeks at home before feeling human. Laparoscopic patients walk out in 3-5 days, back at desk within 2-3 weeks. Bills don’t stop because you had surgery. That time gap costs real money.
- Blood loss: Camera magnifies everything so surgeon sees better, cuts less, cauterizes faster. Blood loss drops 40-60%. Fewer transfusions. Lower infection risk after. Your hemoglobin thanks you.
- Cancer outcomes: Part everyone worries about most. CLASSIC trial, COLOR trial, COST trial. All showed same cancer clearance, same margins, same node harvest, same survival. Colon, rectal, gastric, kidney, gynecological cancers. Equal cure rate. Just less misery getting there.
Surgical team explains which approach fits your tumor when you sit down to review MACS advantages including robotic options that push precision further still.
When Is Open Surgery Still the Smarter Call
- Massive tumors: Anything past 10-12 cm sometimes needs open access because that mass won’t fit through a small port site without risking rupture. Spilling cancer cells during extraction is catastrophically worse than a longer scar. No comparison.
- Adhesion mess: Previous belly surgeries leave scar tissue everywhere inside. Heavy adhesions make laparoscopic navigation dangerous because camera can’t see through tangled tissue. Surgeon might start laparoscopic then convert open halfway if prior operations left too much internal mess to safely work around.
- Vessel invasion: Tumor wrapped around major blood vessels or stuck to neighboring organs sometimes needs hands directly on tissue. Instruments through ports can’t always give the feel needed when you’re peeling tumor off an artery. Millimeters matter there. Literally.
- Surgeon honesty: Laparoscopic cancer surgery has a nasty learning curve. Someone with 500 open cases and 10 laparoscopic ones should do what they’re best at on your cancer. Right technique in shaky hands is more dangerous than older technique in confident ones. Ask your surgeon their numbers. Uncomfortable question but your body, your right.
Right choice depends on cancer, body, and surgeon’s honest read of the situation. Read about recovery after cancer surgery to see how surgical method directly shapes your healing.
Why Choose MACS Clinic?
Call +91 8035740000
FAQs
Is laparoscopic surgery safer than open surgery for cancer?
Does laparoscopic surgery remove cancer as completely as open?
Is laparoscopic cancer surgery more expensive?
Can all cancers be treated laparoscopically?
- Minimally invasive cancer surgery outcomes — National Cancer Institute
- Laparoscopic versus open surgery evidence — World Health Organization