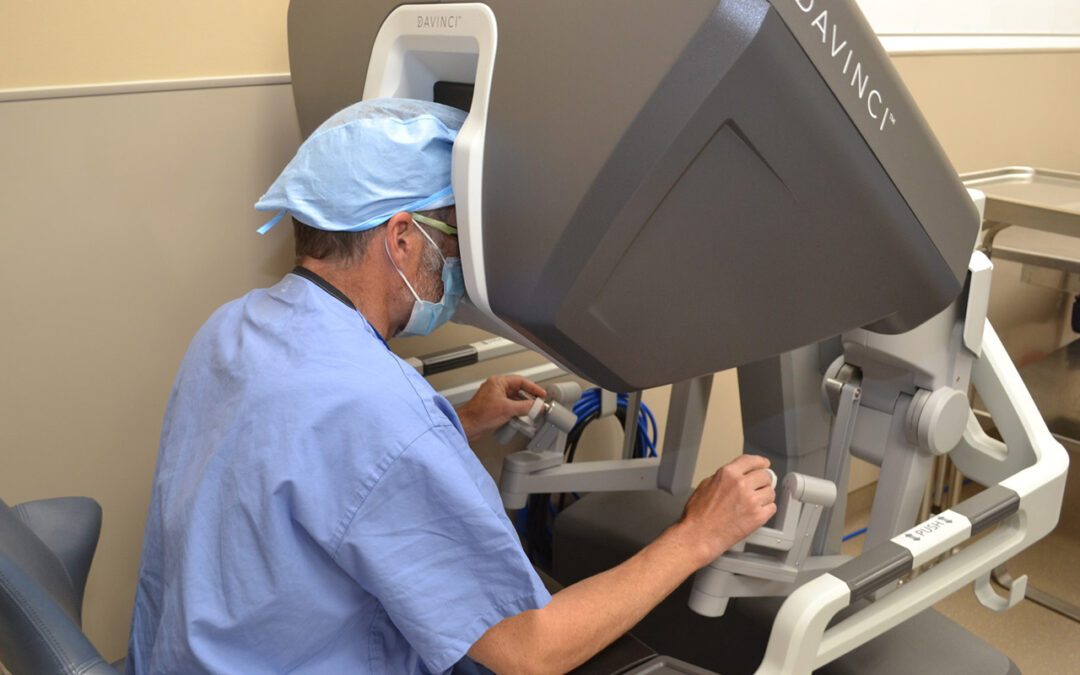
Most early to mid-stage cancer patients with tumors sitting in tight anatomical spaces like the pelvis, prostate, throat, or deep abdomen are ideal candidates for robotic cancer surgery. Robot arms reach angles human wrists physically cannot, which makes it perfect for rectal cancer low in the pelvis, prostate removal, head and neck tumors, and gynecological cancers where precision in a cramped space is the difference between saving an organ and losing it.
According to Dr. Sandeep Nayak, Surgical oncologist in Bangalore, “Robot doesn’t replace the surgeon. It extends what my hands can do in spaces where open surgery would need a much bigger wound to achieve the same result.”
What Makes Someone a Good Candidate?
Not everyone needs the robot. Some cancers do perfectly fine with standard laparoscopic or even open surgery. Robot earns its place when the anatomy is difficult, the margins are tight, and preserving nerves or organs around the tumor matters for quality of life afterward.
- Tumor location: Cancers buried deep in pelvis, behind the breastbone, or wrapped around nerves in the neck benefit most. Robot’s articulating wrists move in 7 directions compared to 4 for laparoscopic instruments. That extra range matters when you’re dissecting tumor off a nerve bundle millimeters away.
- Early to mid stage: Stage I and II cancers are the sweet spot. Tumor is contained, margins are achievable, and the robot’s precision means less collateral damage to surrounding tissue. Stage III can work too depending on location but very bulky tumors pushing past organ walls sometimes need open access.
- Need for nerve preservation: Prostate cancer patients want erectile function preserved. Rectal cancer patients want their sphincter saved. Head and neck patients want their swallowing and voice intact. Robot gives the surgeon magnified 3D vision plus tremor-free movement that makes nerve-sparing technically possible where a human hand alone might not manage.
- Patient fitness: You still need general anesthesia, still need pneumoperitoneum for abdominal cases. Heart and lungs have to handle hours in steep head-down position for pelvic surgery. Fit patients of any age qualify but someone with severe COPD or heart failure may not tolerate the positioning even though the cuts are small.
Surgical team evaluates candidacy based on your scans and fitness when reviewing MACS advantages robotic options during your initial consultation.
Who Should Probably Not Get Robotic Surgery?
Honest answer most clinics won’t volunteer. Robot is a tool not a miracle. Some situations genuinely don’t benefit from it and operating robotically just because the machine is available is expensive ego, not good medicine.
- Very large tumors: Cancer bigger than 10-12 cm needs extraction through an incision anyway regardless of how it was dissected. Using the robot to cut around something that massive then making a 10 cm opening to pull it out defeats the purpose of going minimally invasive in the first place.
- Extensive adhesions: Previous multiple surgeries leave scar tissue everywhere inside. Robot works beautifully in clean tissue. Throw dense adhesions into the mix and the surgeon spends two hours just freeing up space before even reaching the tumor. Sometimes open is faster, safer, and frankly cheaper for everyone involved.
- Widespread metastatic disease: If cancer has scattered across multiple organs the robot isn’t adding value over palliative approaches. Precision dissection matters when you’re trying to cure. When the goal is symptom control, simpler methods work just as well without the robotic price tag.
- Surgeon inexperience: Robot amplifies skill. Also amplifies mistakes. A surgeon with 20 robotic cases shouldn’t be doing complex pelvic dissections robotically yet. Learning curve is steep and your tumor isn’t a training ground. Ask how many they’ve done. Uncomfortable question but you deserve the answer.
Right tool for the right case with the right hands behind it. Read about laparoscopic vs open surgery to understand how robotic fits into the bigger picture of surgical options.
Why Choose MACS Clinic?
Dr. Sandeep Nayak pioneered robotic cancer surgery in India and has thousands of cases behind him across prostate, rectal, head and neck, thyroid, and gynecological cancers. MACS Clinic was purpose-built for this work. Not a general hospital that bought a robot last year. A cancer surgery center that’s been doing this since before most places knew what da Vinci meant.
Team here won’t recommend robotic just because the machine is sitting in the next room. If your cancer does better with laparoscopic or even open approach they’ll say so. Because picking the right method for your specific tumor is the job. Selling you on the fanciest tool isn’t.
Call +91 8035740000 to book your consultation.
Book your consultation for cancer treatment at MACS Clinic, Bangalore.
FAQs
Is robotic cancer surgery better than laparoscopic?
For deep pelvic and confined-space tumors yes. For others the difference is minimal.
How long does robotic cancer surgery take?
Usually 2-4 hours depending on cancer type and complexity.
Is robotic surgery more expensive?
Slightly higher but shorter stay and faster recovery often balance the cost.
Does robotic surgery leave scars?
Minimal scarring from 3-4 tiny incisions of 8-12 mm each.
References
- Robotic surgery in oncology — National Cancer Institute
- Minimally invasive surgical techniques — World Health Organization.